|
The Role of Occupational Physicians in Ergonomic and CTDs
Kevin Byrne, MD, MPH
Occupational physicians view Cumulative Trauma Disorders (CTDs) differently from
other physicians, in large part because the concept of illnesses resulting from chronic
work exposure is fundamental to occupational medicine. As early as 1713, Bernardino Ramazzini the "father" of occupational medicine, described
the cumulative effect of silica dust on miners. Four years later, in The Diseases of
Workers, he recognized two primary causes of occupational injury in certain workers:
those resulting from the nature of the substance and from ‘certain violent and irregular
motions and unnatural postures...’ In the early part of this century, occupational
physicians (or, as they were called at the time, industrial physicians), as well as early
industrial hygienists, began documenting the effects of exposure to lead and other heavy
metals. Later, the results of prolonged exposure to solvents and a host of other substances
began to be recognized, investigated, and regulated. In the 1960s, perhaps as no other illness before, asbestosis received increasing attention
as an occupational disease with a dramatically long latency period (40 years). Only in
recent years has the financial impact of asbestosis been eclipsed by our present epidemic
of CTDs. As the pace of assembly and other work increased, and with the widespread
introduction of computers, we began to recognize the insidious effects of chronic
repetition, excessive force, abnormal and static positions, and vibration. Until recently the prevention of these disorders has received more attention from safety
professionals (ergonomists) than physicians. Fortunately, occupational physicians and
nurses are beginning to change their approach, focusing not only on diagnosing CTDs,
and treating people suffering from these disorders, but also trying to intervene to reduce
them. No longer is it acceptable to treat an injured worker without ensuring that the
precipitating causes are reduced or eliminated. In organizations without a medical
department, someone needs to ensure that appropriate ergonomic corrections and
accommodations are made. Traditional medical providers, especially surgeons, generally
think this falls outside the scope of their field. Occupational doctors have a different paradigm of CTDs because of their training in
population-based medicine. They see their clientele as consisting of groups, not merely of
individuals, and this gives them a broader perspective. Many occupational doctors also
have a degree in public health (MPH or MSPH), with its strong curricula in biostatistics
and epidemiology. Credentialing in Occupational Medicine falls under the umbrella of
the Board of Preventive Medicine. The field of occupational medicine is still very small,
with board-certified occupational physicians representing only one of every 600
physicians in this country. Not only is occupational medicine under-represented in medical school curricula (totally
absent in many) , but the entire field of physical medicine is barely touched upon. It is
therefore no wonder that general and family doctors, especially in managed care, look
askance at CTDs. They have not been trained to investigate the causes, recognize the
physical signs, and offer appropriate treatment of these and other soft-tissue disorders.
Additionally, frequently they over-diagnose and over-treat these disorders. What follows
is a brief review of what I see as the most commonly omitted procedures in CTD
diagnosis and management. 1. Conduct an ergonomic evaluation before a medical workup. Not every person with
hand pain has carpal tunnel syndrome. The premature labeling of someone with this
diagnosis can set the stage for disability. The diagnosis should never be given unless a
definitely positive nerve conduction study and electromyogram (EMG) has been
performed and interpreted by a competent practitioner. These tests are performed
prematurely when no search for risk factors and their control has been done. In every
case, a number of risk factors will be discovered by an onsite workstation evaluation.
All too frequently, the treating physician, whether family doctor or surgeon, sends a
suspected CTS case prematurely for nerve study, including nerve conduction velocity
(NCV) and EMG. The former measures any delay in propagation of the nerve impulse,
such as through the carpal tunnel of the wrist. The EMG uses needles placed in muscles
to detect abnormal function. Although they are usually ordered and performed together,
the needle study need not be performed unless the noninvasive nerve conduction study is
abnormal.
I have seen far too many reports concluded with a hedging statement like, "cannot rule
out CTS," or "compatible with CTS." Worse, the specialist performing the nerve
conduction study may feel obliged to "confirm" the diagnosis of the referring physician,
interpreting the study as positive (abnormal) when it is really borderline or equivocal.
This does a great disservice to all parties (except perhaps the surgeon and hospital).
Before initiating a medical workup, a trial of proper neutral position bracing at night,
anti-inflammatory medications, and frequent stretching is nearly always indicated.
Like most physiologic characteristics, nerve conduction velocity varies from one
individual to another. Cutoff points are frequently arbitrary and too narrow. Nerve
functioning, like all physiological characteristics, has a range of "normal." Some persons
who have no problem will fall outside this range (the so-called, "false positives").
Borderline cases should have the unaffected side studied for comparison. Unless the
nerve study is clearly abnormal and symptoms and physical examination are consistent, a
diagnosis of carpal tunnel syndrome should be withheld. Many patients today equate that
diagnosis with severe disability.
If the nerve study is abnormal, the report should include whether it is acute or chronic,
and whether mild, moderate, or severe. After all, why perform the test, which is
uncomfortable and expensive, if surgery is not being considered? Unfortunately, these
crucial details are usually missing. Knowing the extent and duration of the problem will
influence treatment decisions.
Bottom Line: Do not perform nerve studies unless the causes have been investigated,
alleviated, and initial general treatment measures have failed. Do the testing if it will
influence treatment decisions and ensure that the maximal amount if information is
obtained.
2. Use regional diagnoses instead of over-diagnosing. The pressure to make a specific
diagnosis should be resisted. It is perfectly acceptable, in my opinion, to use a regional
diagnosis such as "hand pain" or "shoulder pain" as a working diagnosis, especially
initially. A given patient with a CTD is likely to receive a different diagnosis from every
doctor that she or he sees, especially in today’s managed care environment. When a
patient is initially told he or she has wrist overuse syndrome and the next week is given a
diagnosis of De Quervain’s tenosynovitis, the result is a breakdown in confidence in the
medical profession — even though these terms are essentially the same. A natural
reaction is to think, "They don’t know what is wrong with me." This in turn leads to
discouragement and concern for the injured person’s future prognosis and career.
Another reason to embrace regional diagnoses is to enable outcome studies. How can we
ever expect to compile our collective experiences with treatment regimens when we all
use a different term for the same, or essentially the same, condition? More than 50
different medical terms are used to describe the typical case of low-back pain. We will
never be able to assess the efficacy of the many types of physical therapy, for example, if
we cannot agree on a common term. Bottom Line: Use regional diagnoses such as "hand pain," "elbow pain," and "shoulder
pain" instead of the myriad of specific diagnoses that serve only to bolster an impression
of the physician’s diagnostic acumen. 3. Avoid over-treatment: Mobilize, don’t immobilize. Braces for CTDs should be
properly selected and carefully used. Even today, many persons with CTDs are told to
use a brace at work. The misunderstanding that theses injuries arise principally from
repetitive motion has generated a misguided notion that immobilization is curative. Lack
of motion, such as static posture, is much more common as a precipitating factor. Hours
spent reaching forward for the mouse or keyboard, staring at the monitor, holding the
wrists, thumbs or little fingers up high, all are greater contributors to injury than even the
most rapid keyboarding with proper technique. There are times when a wrist brace is useful, but almost never when at the keyboard.
Carpal tunnel sufferers, in particular, are much more comfortable in a brace while
sleeping. These braces generally have their stabilizing element along the back of the hand
and forearm and keep the wrist in a neutral position. I still occasionally see patients who
have been given or have self-prescribed a wrist brace that not only increases pressure in
the carpal tunnel by a metal stay along the palmar aspect of the wrist (at the base of the
palm), but also forces the wrist into an extended (upward) position—which also increases
pressure within the carpal tunnel. (See image.) 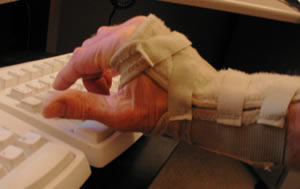
If the improper wrist position has not been corrected, wrist braces can create another
problem. If VDT workers tend to hold their wrists up when keying (which is the most
common position), they will tend to "fight" the brace, which is restricting this motion.
The result is often a pain along the outer aspect of the elbow (commonly known as
"tennis elbow"). This location, called the lateral epicondyle, is the origin of the muscles
that extend the wrist upwards. As a final example, a sling for a shoulder strain is almost
always inappropriate. Unless discarded quickly, it will lead to stiffness, loss of motion,
and weakness.
Bottom Line: Motion is essential for normal activity and for resolution of CTDs.
4. Avoid excessive restrictions. Vague, global restrictions such as "no repetitive use of
the arms" or "no keyboarding" are easy for the medical provider to prescribe but
counterproductive and irresponsible. Although movement may need to be moderated and
abnormal positions corrected, in general it is therapeutic. In fact, movement is essential
for recovery. Excessive restrictions set the stage for "off duty" status, displacement from
usual routines and family roles, and a progressively downward spiral of fear,
discouragement, anger, depression, and disability. Instead, the medical provider should set realistic restrictions based on the patient’s job
duties and objective reckoning of their ability. An accurate history may reveal that the job
requires intermittent rather than continuous keyboarding. This may be permitted in all but
the severest cases. Objective testing is available by most physical and occupational
therapy departments. Some can verify the level of keyboarding ability by observation and
monitoring of the heart rate. (Pain will lead to a rise in heart rate.) Much more effective are restrictions that displace the precipitating causes. Examples:
"Gentle stretching for about 3 minutes every half hour," "stand up or walk about once
every hour," "must use proper keyboarding technique," "limit keyboarding to 30 minutes
per hour," or "must adjust workstation correctly." Unless the case is far advanced, these
restrictions not only lead to recovery, but alleviate the underlying cause of the problem. It
is rare for a substantiated CTD sufferer to have correct workstation adjustment and use
correct keyboarding technique. Personally, I have never seen this. 5. Surgery should be the last and seldom-utilized resort. The most egregious
mismanagement of CTDs occurs when a person is operated upon without sufficient (or
any) documentation that surgery is necessary, or without attempting to understand and
mitigate the risk factors. Sometimes this disregard for precipitating causes extends to the
postoperative period, when patients are told they are "cured" and then returned to the
same environment that caused the condition. At other times they are advised never to use
a keyboard again, effectively condemning them to career disaster, lifelong disability, and
depression. I have seen this happen far too often. Bottom Line: Carpal tunnel syndrome and other CTDs are not surgical problems, they are
ergonomic problems. Fortunately, there are very effective ergonomic solutions, especially
when initiated early. If primary prevention measures are taken—that is, before the
development of symptoms—essentially all of these problems could be eliminated from
the workplace. Although surgery may be indicated, it should be rare and cannot be
successful independent of the ergonomic solutions.
|

